ARTICLE OVERVIEW: Hydrocodone withdrawal is like a bad flu. Symptoms include nausea, vomiting, and fever. More on what to expect during withdrawal here.
TABLE OF CONTENTS
- Psychoactive Effects
- Physical Dependence
- Duration
- Common Symptoms
- Protracted Symptoms
- Tapering
- Treatment
- Medications that Help
- Detox at Home?
- Safety
Psychoactive Effects
Hydrocodone is a part of the opioid family of analgesic (painkiller) drugs, derived from codeine. Its use was approved by the FDA in 1943. [1] But how does hydrocodone work?
When you take hydrocodone, it suppresses the pain receptors in the brain and the spinal cord, and slows overall body responses. It also acts on opioid receptors in the central nervous system to trigger euphoria, a feeling of extreme well-being. This is why when you are on hydrocodone you can no longer feel pain and/or can feel a hydrocodone high.
But you also run the risk of developing a hydrocodone physical and psychological dependency and high tolerance levels anytime you take hydrocodone regularly for more than a couple of weeks. This is why the DEA monitors the sales and distribution of hydrocodone, as it falls under a Schedule II drug, classified in the Controlled Substances Act. [2]
Physical Dependence
Dependence is a condition caused by chronic use of a psychoactive drug, in which abrupt or gradual drug withdrawal causes unpleasant physical and psychological symptoms. Drug tolerance is a pharmacological concept describing a person’s reduced reaction to a drug following its repeated use. In other words, people who are hydrocodone-tolerant need to take more of the drug ore often to achieve initial therapeutic effect.
When you develop dependence on hydrocodone AND you decide to stop taking hydrocodone, you will quickly feel the withdrawal symptoms of the medication. Hydrocodone withdrawal symptoms occur as your brain and body seek homeostasis after you stop taking the pain killer. Usually, these symptoms begin right when you’re expecting your next dose. Why?
Withdrawal symptoms occur because the body adapts to any drug by adjusting chemically triggered processes. Drugs like hydrocodone deposit chemicals into the brain, “slowing down” the body due to its depressant effects. When this happens over time, your body adapts by “speeding up” processes in order to balance out. Otherwise, you wouldn’t be able to function.
In other words, hydrocodone withdrawal happens when your brain signals the lack of hydrocodone in the system, but the “quickened” processes take time to slow down again.
Duration
Hydrocodone withdrawal symptoms can develop within a few hours of your next, expected dose. In fact, you can expect to feel hydrocodone withdrawal begin shortly after a missed dose. It peaks within 12–48 hours, and subsides over 10–20 days. The degree and time that withdrawal takes, however, can fluctuate given your daily dose frequency and amount.
After about 2 to 3 days, people report intense hydrocodone cravings. However, a level of normalcy returns in about a week. Once you have gone through the physical effects hydrocodone withdrawal, you will have to deal with the psychological craving for the drug. This can persist for weeks or months after you quit. So, you’ll need to learn new habits to kick the need to take it again when stressors arrive.
Common Symptoms
In general, withdrawal symptoms are more intense when your hydrocodone prescription dosage has been high.
There are varieties of symptoms you may experience withdrawing from hydrocodone. Early signs of hydrocodone withdrawal can include runny nose, excessive sweating, shedding tears, yawning, dilated pupils, and increased temperature.
Later signs of hydrocodone withdrawal include: loss of appetite, nausea, vomiting, diarrhea, a continual or recurrent inclination to evacuate the bowels, goose flesh, weakness, increased blood pressure and pulse, agitation, restlessness, and severe muscle and bone pain.
The most commonly reported symptoms of hydrocodone withdrawal include:
- Cold flashes with goose bumps.
- Excessive yawning or sneezing.
- Extreme drowsiness.
- Diarrhea.
- Insomnia.
- Involuntary leg movements.
- Mood changes.
- Muscle and bone pain.
- Sweats.
- Strong drug craving.
Protracted Symptoms
Acute opioid withdrawal is followed by a protracted withdrawal phase that lasts for up to six months. In fact, some symptoms can continue in the weeks and months after acute hydrocodone withdrawal. These symptoms are called protracted, or post-acute withdrawal symptoms (PAWS). Often, PAWS may require additional medical help, as they can be treated with a combination of medications and talk therapy.
Hydrocodone PAWS are characterized by a general feeling of reduced well-being and strong cravings for opioids. This craving often leads to relapse to opioid use. To reduce the risk of relapse, patients should be engaged in psychosocial interventions.
The most commons hydrocodone PAWS include:
- Anxiety.
- Cravings.
- Depression.
- Mood swings.
- Trouble sleeping.
Tapering
In many cases, symptoms can be made less severe or intense when you gradually reduce doses over time. “Tapering” is the medical term for slow dose reduction over time. Consider tapering to a reduced dosage anytime you:
- Are taking dosages ≥ 50 morphine milligram equivalents /day without benefit.
- Are taking hydrocodone at the same time you’re benzodiazepines.
- Do not have clinically meaningful improvement in pain.
- Experience overdose.
- Experience serious side effects.
- Shows signs of addiction.
- Show signs such as confusion, sedation, or slurred speech.
- Want to quit for good.
What guidelines can you follow? The CDC Pocket Guide for Tapering Opoids for Chronic Pain suggests that a decrease of 10% of the original dose per week is a reasonable starting point. Some people who have taken painkiller narcotics for a long time might find even slower tapers 10% dosage decrease per month easier. [3]
Do not reverse the taper! This can cause overdose. However, the rate may be slowed or paused while monitoring and managing withdrawal symptoms. Once the smallest available dose is reached, the interval between doses can be extended and hydrocodone may be stopped when taken less than once a day.
Treatments
Withdrawal is the necessary next step to getting hydrocodone out of your body. Nevertheless, there is no reason that you should suffer during detox. In fact, painful withdrawal decreases likelihood that you stop taking hydrocodone in the long term. The educational, emotional, and psychological support of medical professionals who know about withdrawal is critical!
Doctors typically treat the first stage of withdrawal with medicines that address acute detox symptoms.
What medicines are used in cases of extreme drug dependence? Doctors commonly use methadone, buprenorphine, or naltrexone to make withdrawal more manageable. Many times, clonidine can be prescribed for symptoms. Anti-diarrheal agents are given when appropriate. Doctors also offer other medications to help treat depression or anxiety, when needed. Long-term opioid substitution therapy may be recommended on some cases.
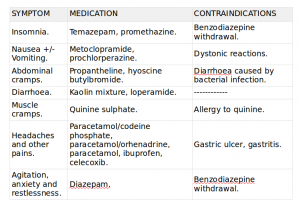
For specific symptoms the following table resumes their treatment:
Medications that Help
Buprenorphine: This is the best opioid medication for management of moderate to severe opioid withdrawal. It alleviates withdrawal symptoms and reduces cravings. Because of its pharmacological action (partial opiate agonist), buprenorphine should only be given after the patient begins to experience withdrawal symptoms. Buprenorphine should be used with caution in patients with:
- Respiratory deficiency.
- Urethral obstruction.
- Diabetes.
Clonidine: The first line of treatment to reduce symptoms is Clonidine. Clonidine is an alpha-2 adrenergic agonist. It can provide relief to many of the physical symptoms of opioid withdrawal including sweating, diarrhea, vomiting, abdominal cramps, chills, anxiety, insomnia, and tremor. It can also cause drowsiness, dizziness and low blood pressure. Clonidine can also be used in conjunction with symptomatic treatment as required. It should not be given at the same time as opioid substitution. Blood pressure and heartrate monitoring should be taken into account.
Methadone: This medicine alleviates opioid withdrawal symptoms and reduces cravings. Methadone is useful for detoxification. Methadone should be used with caution if the patient has:
- Respiratory deficiency.
- Acute alcohol dependence.
- Head injury.
- Treatment with monoamine oxidase inhibitors (MAOIs).
- Ulcerating colitis or Crohn’s disease.
- Severe hepatic impairment.
Anyone who goes through withdrawal should be advised that they are at increased risk of overdose due to reduced tolerance.
Monitoring
People should be monitored regularly (3-4 times daily) for symptoms and complications during hydrocodone detox. The following Short Opioid Withdrawal Scale is a useful tool for monitoring withdrawal. In fact, a few main symptoms can and should be assessed 1-2 times daily. These include:
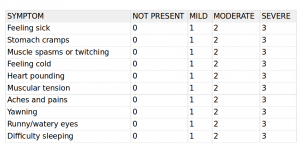
Add scores for total score:
Compare total score to table below to guide withdrawal management.

It is important to drink at least 2-3 liters of water per day during withdrawal to replace fluids lost through perspiration and diarrhea. Also, vitamin B and vitamin C supplements can help.
Detox At Home?
So, can you detox from hydrocodone safely at home?
The safest way to detox from hydrocodone is under medical supervision.
Still, it is possible to detox at home if you have just started taking it, are in good general health, and have a support system. Be sure that you know what to expect during detox and for how long. You can use this timeline for hydrocodone symptoms for a week-by-week snapshot of most cases of detox.
However, some people do not qualify for detox at home. If have taken hydrocodone for more than a few weeks, medical supervision is strongly recommended to manage tapering, because drug cravings make it harder to deal with withdrawal symptoms. Further, if you are taking other medications or are in poor health, medical detox will be a necessary.
Safety
Most experts recommend that you treat withdrawal from hydrocodone under medical supervision. Why? To make sure that you have the support you need to help you to combat the withdrawal symptoms.
Serious problems can appear during the withdrawal process such as recidivism and overdosing with very dramatic complications such as respiratory deficiency and death.
It is also recommended that you be monitored by a physician especially if they are already in charge of your doses. By slowing tapering off hydrocodone, you can minimize the intensity and variety of withdrawal symptoms that you feel.
More Questions?
If you still have any question about coming off prescription meds safety, you are not alone! Feel free to call us or leave us a question in the comments section at the end. We´ll try to answer all hydrocodone withdrawal questions as promptly as we can! Privacy guaranteed.











Related Posts